It may sound like a contradiction, but it’s true. Using HITEKS to power the native Epic Note Editor workflows supports an Epic First Strategy. If your hospital system hasn’t done so already, it will likely decide on using tools that are natively embedded and power Epic’s core functionality, including Diagnosis Aware Notes, CDI and Coding WorkQueues, and other Foundation features.
But adopting an Epic First Strategy isn’t just about technology consolidation, it’s about philosophy. It’s a commitment to building workflows that meet clinicians where they already are, rather than asking them to context-switch between platforms, learn new interfaces, or manually reconcile data across systems. Every additional tool that lives outside of Epic is another source of friction. And in a clinical environment, friction has a cost, measured in time, in errors, and ultimately, in patient outcomes.
That’s why health systems that have embraced an Epic First approach consistently report stronger adoption rates, more consistent documentation, and better alignment between clinical and administrative teams. When the tools clinicians rely on are seamlessly woven into the platform they use every day, the entire organization benefits, from the frontline provider to the billing department to the C-suite.
The goal is to reduce provider burden by simplifying the User Interface screens and workflows so that all of the intelligence from analytics takes place seamlessly and presented within Epic with the fewest clicks possible. HITEKS makes that vision a reality, not by replacing Epic’s native capabilities, but by supercharging them..
How HITEKS works with Epic’s Diagnosis Aware Notes (DAN) to save physicians time with the problem list and get more accurate results
In today’s day and age, it may be easy to forget, but words still matter. And when you’re a clinician, words can even have a life-or-death importance.
When a patient comes in reporting a specific symptom, it’s easy to see it as an isolated case, but often, they may have a history of issues that need to be analyzed and treated as a whole, part of a patchwork rather than an individual incident.
That’s where precise note-taking and query review comes in. Doctors, nurses, dieticians, occupational therapists and other clinicians can’t be expected to remember and correctly log every detail of a patient’s history or comorbid conditions in a silo. Sometimes, even they need a little prompting from the computerized analysis of the patient’s past and current visit notes, laboratory test results, medication list, flowsheet data and vital signs.
Why do good notes matter for physicians?
Any software and AI-based system that improves note-taking and frees time for patient care is better for clinicians and it’s better for patients. One of the principal issues for practicing clinicians is burnout, how do you manage your administrative tasks on top of all of the one-to-one patient work necessary for any provider?
The answer is, in part, smart automation. CDI Tools like HITEKS’ CAPD360 Insight for Epic NoteReader CDI and Queryless CDI powering DAN help combat physician burnout by automating tasks like chart reviews, clinical note entries and problem list updates. And when providers aren’t sure or have a question, the system sends real-time prompts and corrections that ‘nudge’ them to choose a more accurate and compliant diagnosis, which helps the entire chain of healthcare administration.
The ripple effect of better documentation extends far beyond any single encounter. When physicians trust that their documentation tools are working with them, not against them, they can redirect their energy toward what matters most: meaningful patient interaction. Reducing the mental overhead of administrative tasks doesn’t just improve job satisfaction; it directly correlates with lower rates of clinical errors, improved diagnostic clarity, and better care team communication. In a healthcare environment where every minute counts, that kind of efficiency isn’t a luxury, it’s a necessity.
Why do good notes matter for patients?
Clinicians aren’t the only ones who benefit from automated CDI systems, patients do as well. With more accurate documentation on the front end, patients’ claims are more frequently coded correctly the first time, making for fewer denied claims and accurate reimbursements from insurance providers. In addition, clinical validation of stated diagnoses which get high scrutiny from payers, such as Sepsis, Encephalopathy, and Acute Kidney Injury, can justify the diagnosis with explicit criteria that can be audited from the patient’s record.
Patients can also fare better with clinical outcomes with real-time Epic-embedded CDI systems. When an entire patient’s history is available for Quality and CDI Specialists to review and justify querying a provider, with the click of a button in the EHR, they’re able to better see the whole picture in a timely manner. Patient Safety Indicators (PSIs) and Hospital Acquired Conditions (HACs) are also identified and documented more accurately, resulting in a patient-first culture that ensures Primum Non Nocere, the Latin medical concept taught in medical education programs which promotes ‘First Do No Harm.’ Catching these conditions early-on enables quality-driven organizations to intervene and address the safety concern before it escalates.
Beyond safety indicators, there’s another dimension to consider: patient trust. When a clinical team arrives at the bedside with a complete, up-to-date picture of a patient’s history, without the need to ask repetitive questions or flip through disconnected records, patients notice. That seamless continuity of care strengthens the provider-patient relationship and contributes to better health outcomes, higher satisfaction scores, and a stronger reputation for the health system as a whole.

How HITEKS works with Epic’s Diagnosis Aware Notes to save you time and get more accurate results
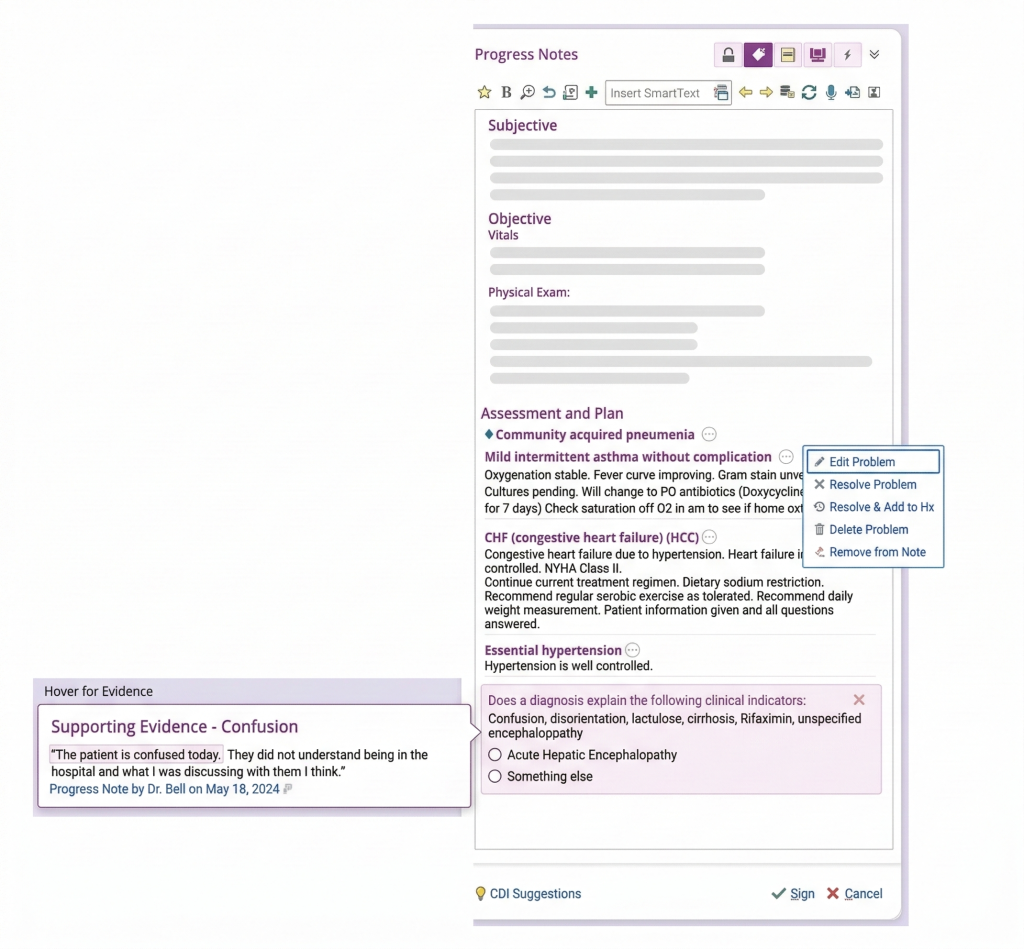
HITEKS’ CDI platform supports both physicians directly and CDI staff indirectly and is seamlessly integrated into Epic’s newest documentation and problem list synchronization feature, Diagnosis Aware Notes, available as an Epic Smartlink that powers the Assessment and Plan section of the visit and progress note. This helps save time in documentation integrity and delivers targeted CDI Queries within each patient assessment. More importantly, HITEKS’ documentation integrity system keeps your patient’s problem list up-to-date, ensuring efficient and accurate continuity of care.
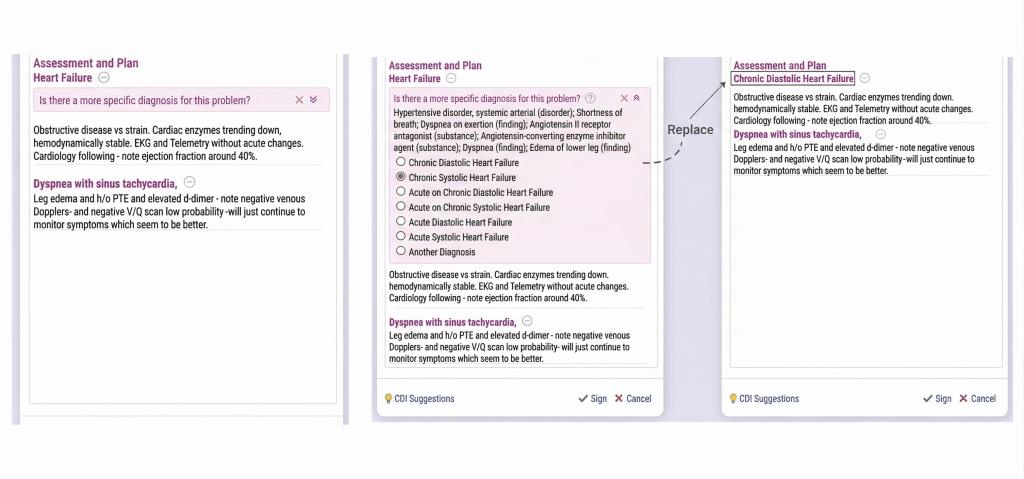
Physicians can use Diagnosis Aware Notes as a condensing and analyzing tool, helping to mitigate the overwhelming review activity that sometimes comes with too many notes and too much data that aren’t immediately placed in a useful context. Powering DAN is the result of designing the system with Epic, enabling an embedded, advanced navigation in Notes, and prompting clinicians to review additional information, like the patient’s organ system history and relevant laboratory test results and imaging findings, which can result in an updated diagnosis and documentation of what they did to Monitor, Evaluate, Assess and Treat (M.E.A.T. criteria) the patient, all with the click of a button.
For CDI specialists, the integration means less time chasing physicians for clarifications and more time focused on high-value review. The workflow is intuitive: rather than sending manual queries through separate channels and waiting for responses, CDI teams can interact with providers directly within the Epic environment, in context, in real time. This tighter feedback loop means queries get resolved faster, documentation gaps get closed sooner, and the data reflected in the patient’s record is more complete, and more defensible, at the time of billing and audit.
Here’s what makes HITEKS different
CDI tools may seem all alike, but HITEKS really does offer something a cut above. Our CDI systems have some of the largest diagnosis libraries in the industry, built and refined from our clients over time, and can capture between 80 to 90% of all diagnoses relevant to the inpatient (and soon ambulatory) visit. Physicians also report how easy it is to use HITEKS’ products, especially since they are natively embedded into Epic’s features.
And when it comes to accuracy, the numbers speak for themselves. While many nudge tools operate at between 65 to 80% accuracy, HITEKS’ automated clarifications are between 95 and 100% accurate, meaning clinicians don’t have to waste time fact-checking prompts or second-guessing suggestions. Every recommendation that surfaces in the workflow is one they can act on with confidence.
That level of precision also matters at the organizational level. When hospital systems can rely on consistent, high-accuracy documentation across their entire provider network, they see measurable improvements in case mix index, compliance audit readiness, and overall revenue integrity. HITEKS isn’t just a tool for individual physicians, it’s a scalable solution designed to elevate documentation standards across departments, service lines, and campuses.
As healthcare continues to evolve, with increasing regulatory scrutiny, growing documentation complexity, and mounting pressure on clinicians, the case for intelligent, embedded CDI solutions has never been stronger. HITEKS is built for exactly this moment.
Want to learn more about what HITEKS is doing to help reduce physician burnout and improve patient outcomes? Click here to read more about our real-time CDI tools in Epic.



