In Clinical Documentation Integrity (CDI) programs, MEDPAR (Medicare Provider Analysis and Review) data and quality data analytics are invaluable tools. These resources offer detailed records of Medicare patients’ diagnoses, procedures, and healthcare service utilization. The analytics also track to other payer reimbursement systems like Medicaid, other State Reimbursement Programs, and Private Insurers.
In this article, we will explore the significance of MEDPAR data and quality data analytics and how they contribute to identifying potential gaps in patient care, ensuring accurate reimbursement, and satisfying quality metrics.
Leveraging MEDPAR Data for Revenue and Quality Metrics
MEDPAR data serves as a treasure trove of information that CDI teams can utilize for numerous purposes. It enables the identification of discrepancies between documented diagnoses and coded information, ensuring accurate coding to prevent undercoding or overcoding. Aligning coding practices with MEDPAR data leads to appropriate reimbursement.
Moreover, analyzing MEDPAR data helps CDI teams track quality metrics such as readmission rates, complications, and mortality rates, facilitating a better understanding of care quality and pinpointing areas for decision support to reinforce evidence-based care for both the principle diagnosis and comorbidities.
By identifying trends in MEDPAR data, CDI teams can implement proactive strategies to educate providers and send note inquiries (aka CDI Queries) which can capture the fully specified or forgotten clinical conditions important to the relevant risk models.
Empowering CDI with Quality Data Analytics
Quality data analytics involves the systematic analysis of healthcare data to reveal trends, patterns, and crucial insights concerning patient care and outcomes. In CDI programs, quality data analytics is essential for achieving superior outcomes. By scrutinizing quality data, CDI teams can identify areas where patient care can be improved, addressing the gaps to enhance patient safety, satisfaction, and overall care quality.
Through the analysis of documentation practices, CDI teams can pinpoint documentation gaps that might compromise the accuracy and completeness of patient records. By leveraging these insights, CDI teams can create targeted queries and improve overall documentation practices. The benchmarking of hospital performance against industry standards and best practices provides CDI teams with a valuable means of setting performance goals and measuring the effectiveness of CDI efforts. Additionally, quality data analytics supports compliance with regulatory requirements and reporting obligations, ensuring that accurate and comprehensive documentation is in place to adhere to reporting standards and avoid penalties.
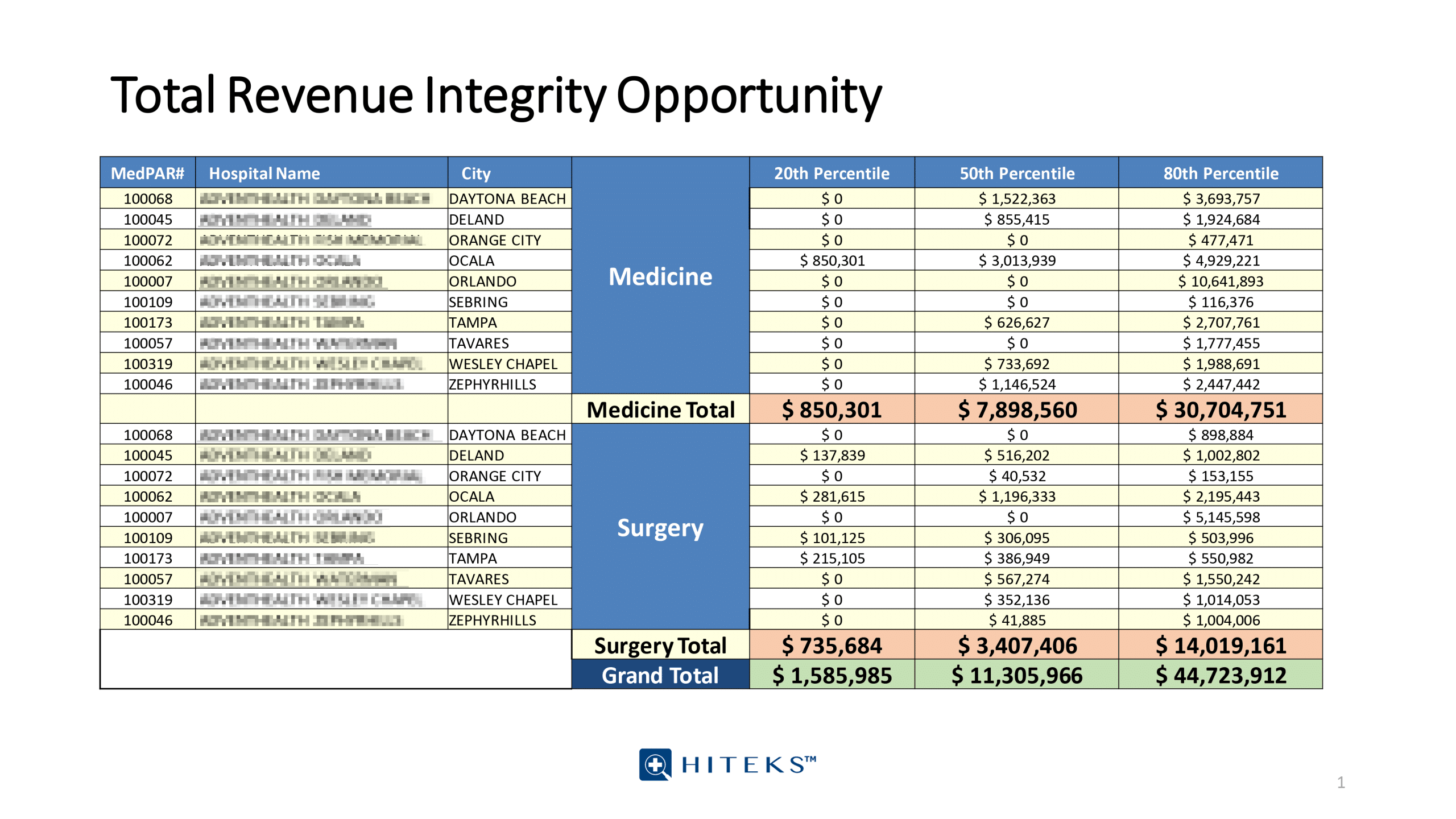
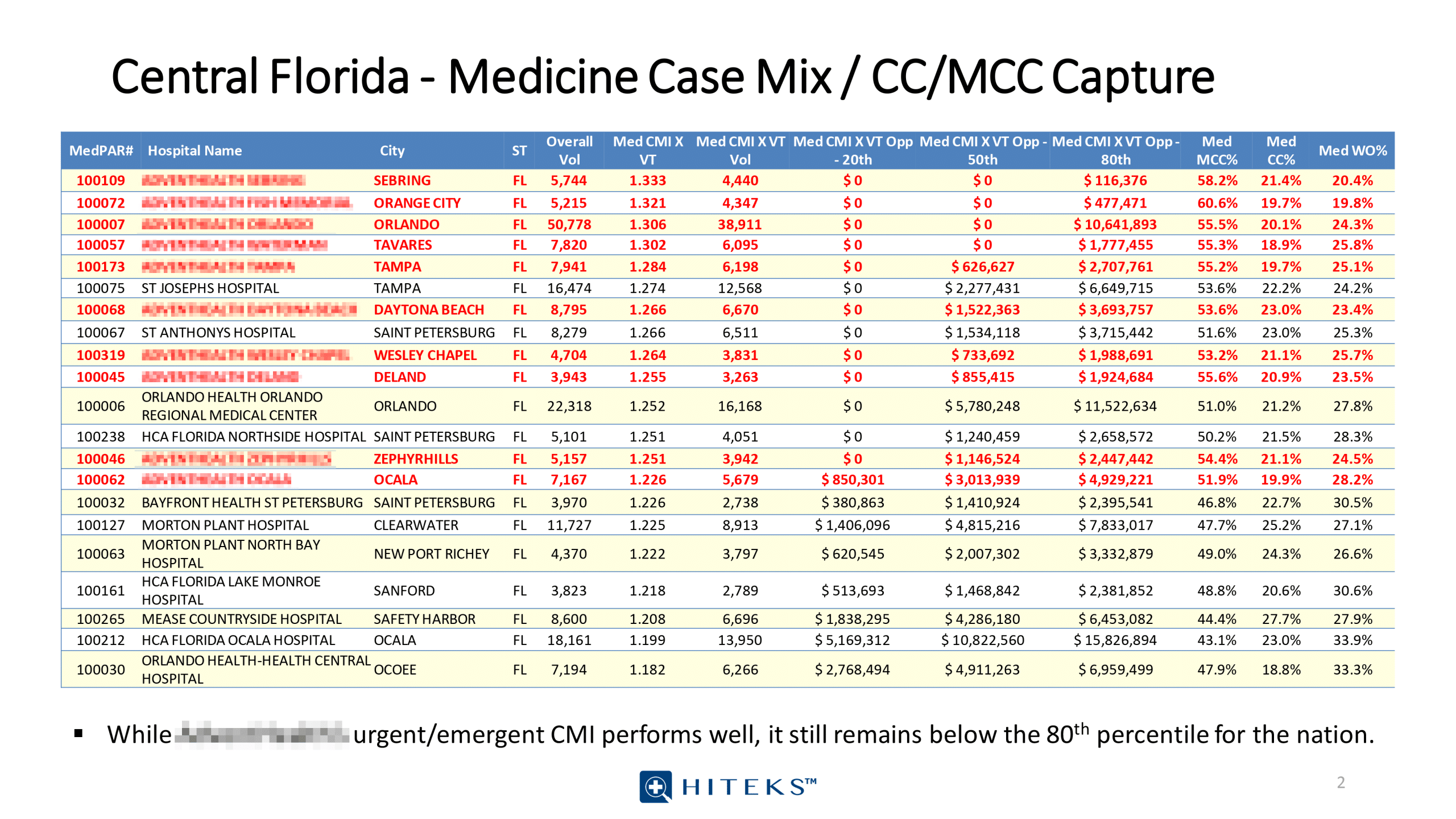
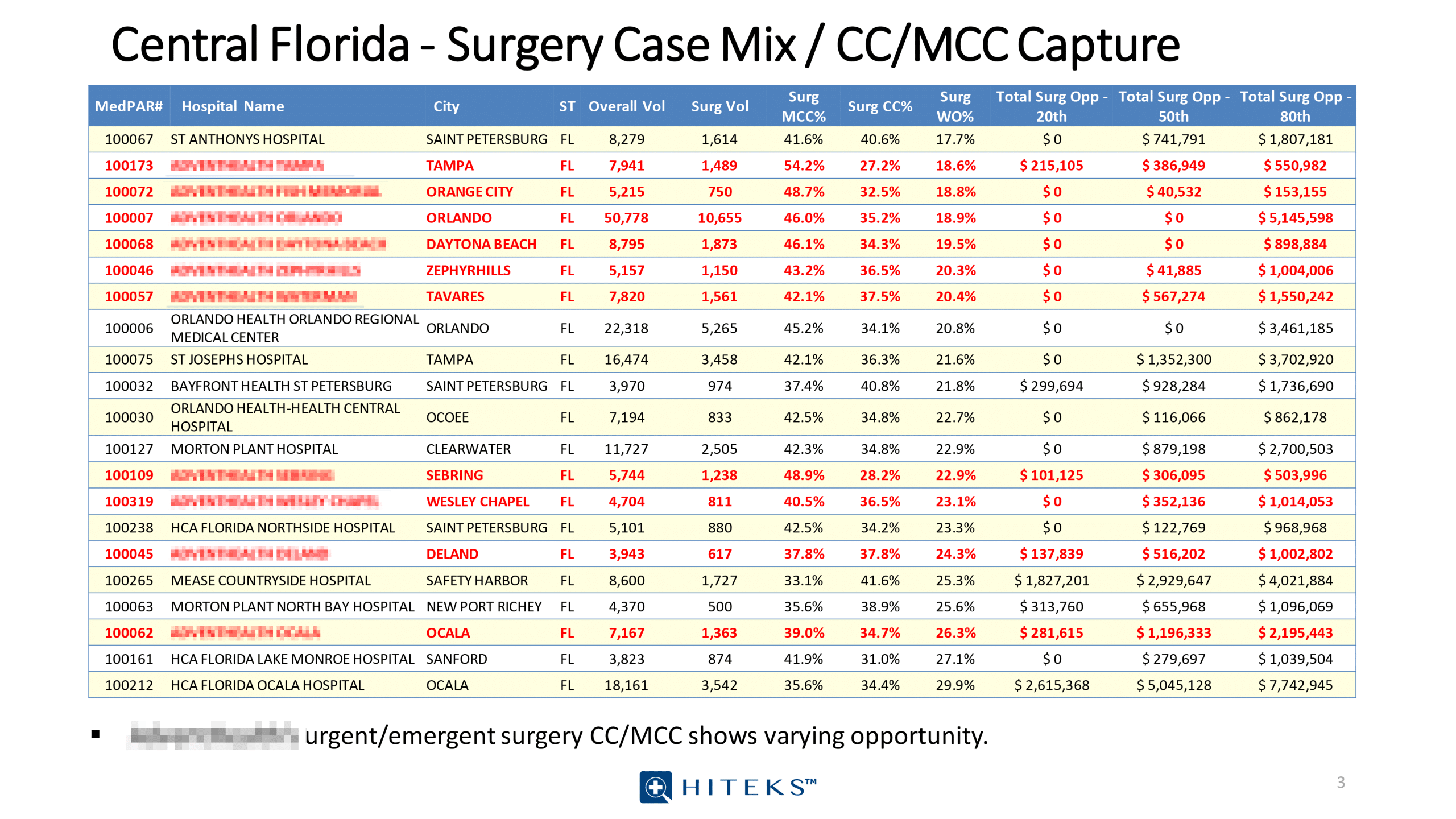
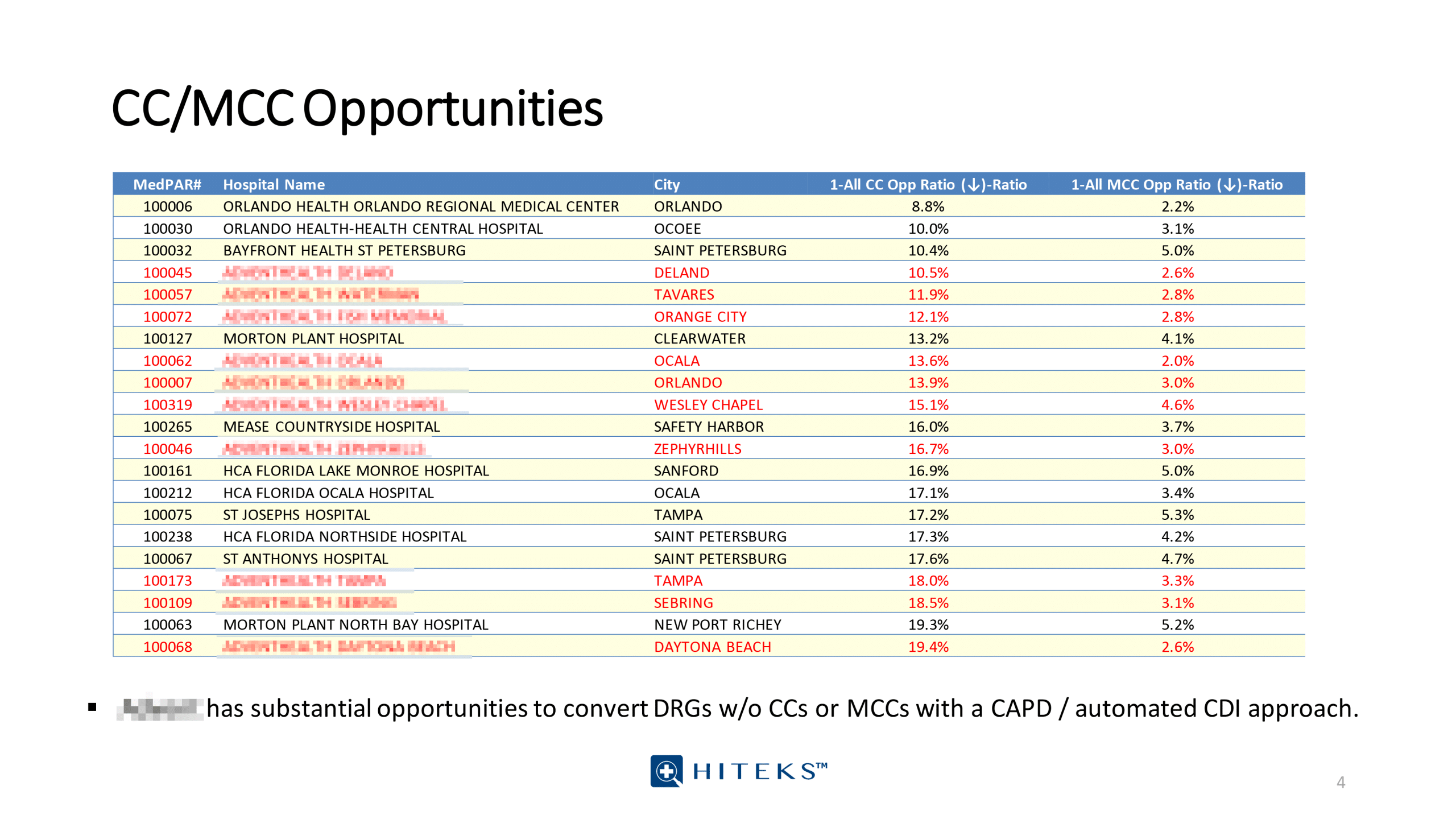
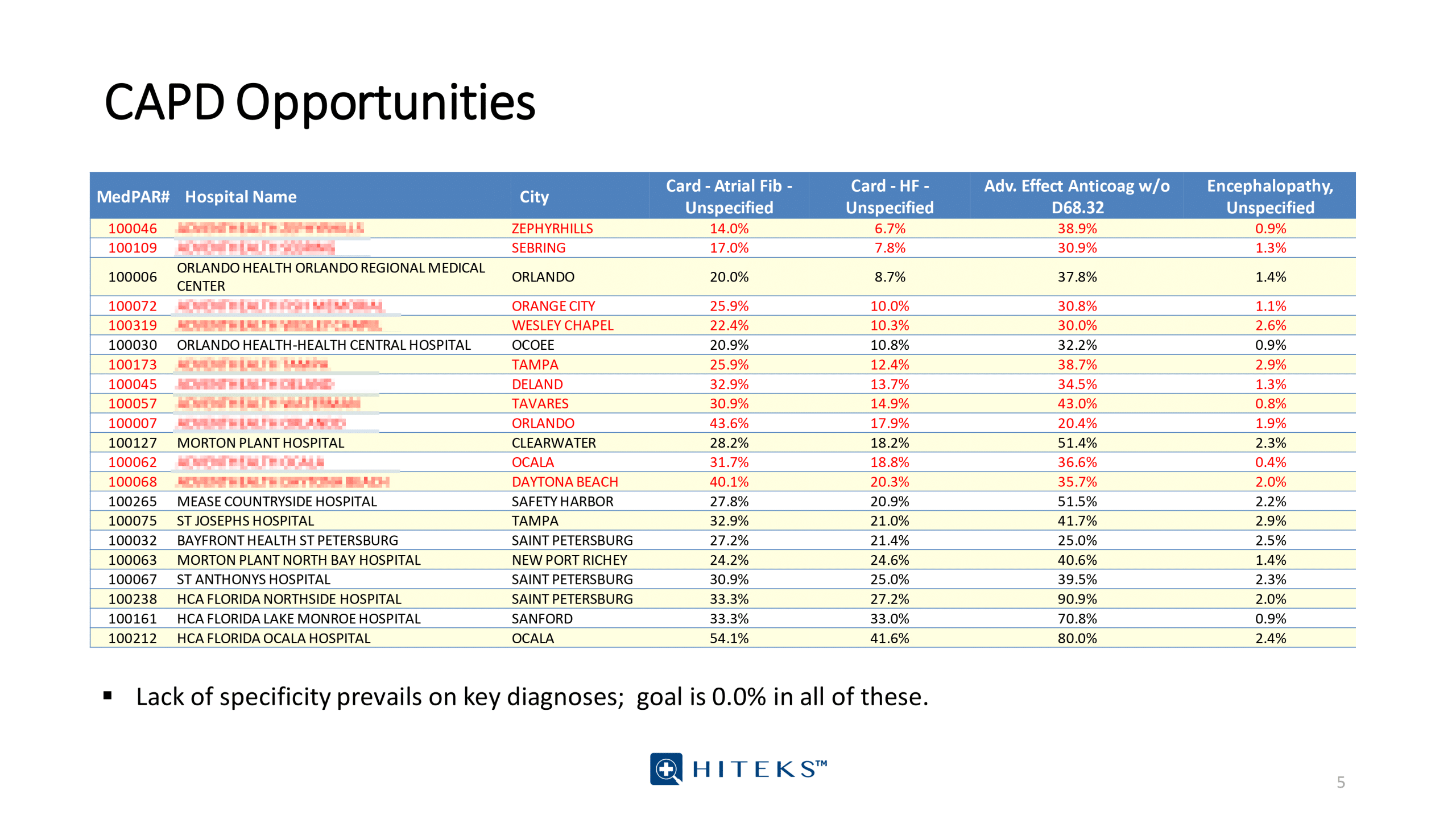
MEDPAR data and quality data analytics into CDI Workflows
By incorporating MEDPAR data and quality data analytics into CDI processes, healthcare organizations can significantly enhance patient care, optimize reimbursement, and meet regulatory requirements. These insights enable CDI teams to continually improve coding practices, drive proactive strategies for clinical decision support, and deliver high-quality care to patients.
At HITEKS, we provide comprehensive data access, empowering CDI teams to identify trends, measure performance, and make informed decisions for improved patient outcomes and elevated care quality. Through the harnessing of MEDPAR data and quality data analytics, HITEKS empowers healthcare organizations to optimize reimbursement, compliance, and contribute to a healthier and more efficient healthcare ecosystem.
Discover how HITEKS can transform your CDI processes and elevate the standard of clinical coding and patient care.



